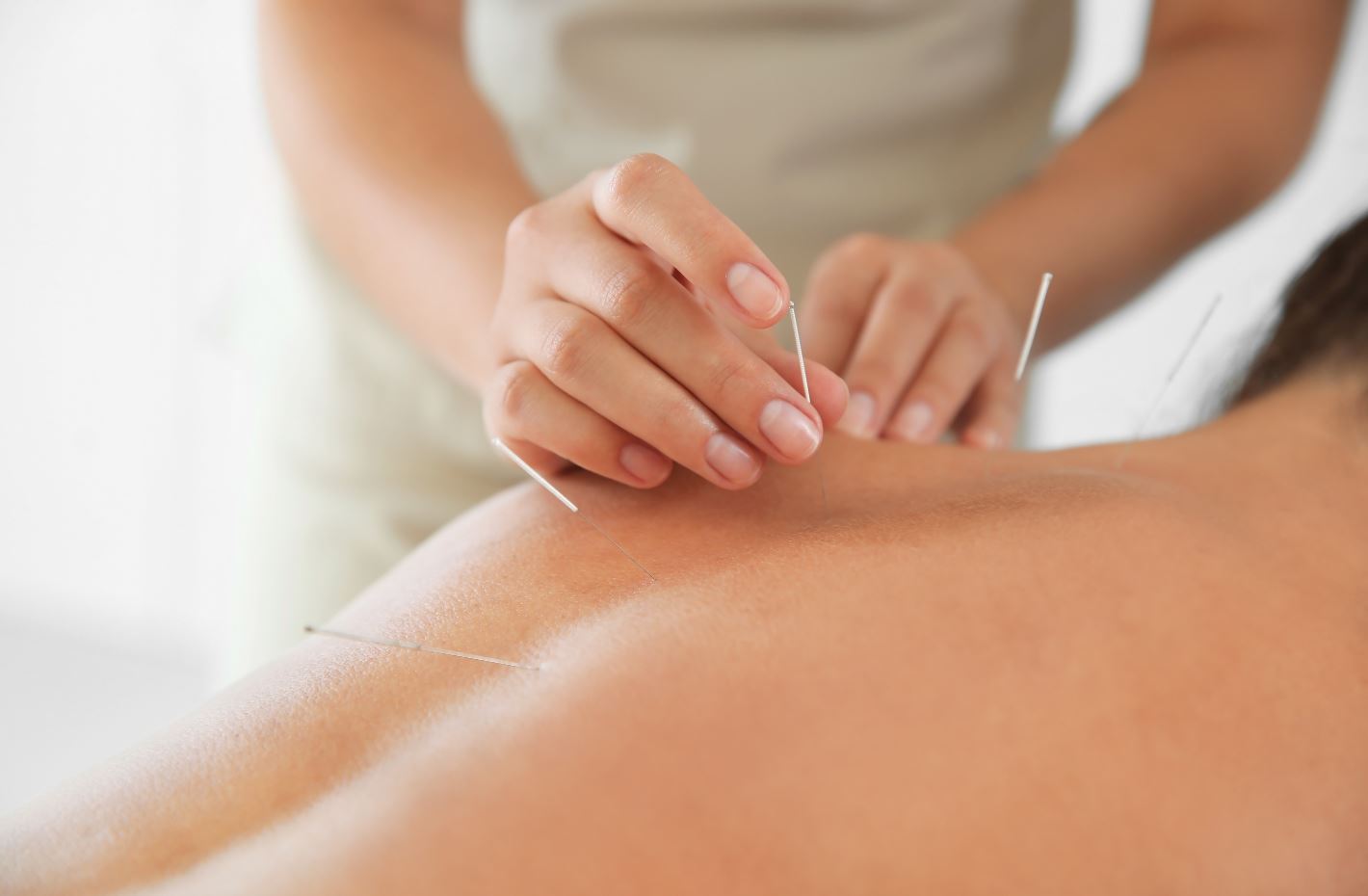
Hawthorn Healing Arts - Naturopathic Medicine and Services
At Hawthorn Healing Arts Center we know that the path to wellness often involves many trails, so we offer a wide array of healing arts that complement, support and enhance each other. All of our clinicians and specialists work together as a team to bring you optimal wellness, holistically.